Dementia Gardens
Purpose & Definition.
Dementia gardens are gardens designed to specifically meet the needs of dementia patients. The gardens are usually located in aged-care facilities and they should take into account both the physical and mental symptoms of individuals at each stage of the disease, as listed in the previous section.
The goal of treatment gardens for Alzheimer patients according to Zeisel and Yson, is ‘to create a well-designed environment with good planning and medical and social management to reduce symptoms and ease the burdens on family members or caregivers.’
But why create gardens for dementia patients in the first place? What do they offer and how should this best be achieved? What are the principles of a well-designed garden for dementia patients?
Benefits of Dementia Gardens.
According to Kaplan (1995), nature is restorative and has healing powers.
This is true for both those afflicted by dementia, but also for well individuals who seek to escape the pressures of everyday life by interacting with nature.
Research indicates that physical and visual access to nature can have the following positive impacts in individuals with and without dementia:
Helps people recover from illness quicker
Reduces stress and lowers blood pressure
Helps a person maintain circadian rhythms
Aids in the natural absorption of vitamin D when exposed to sunlight for brief periods of time, which is important for maintaining strong bones.
In addition to this, the benefits of a garden as a place of quiet beauty and mental rejuvenation have been shown to increase with age and have been established for people with dementia specifically.
Gardens and outdoor environments are being increasingly reintroduced as important support tools in the care, management and contribute to the quality of life of people with dementia.
Some of the benefits for dementia sufferers include:
Enjoyable form of exercise
Increases levels of activity and maintains mobility and flexibility
Encourages use of motor skills – walking, reaching, bending, planting seeds and taking cuttings
Improves endurance and strength
Helps prevent diseases such as osteoporosis
Reduces stress levels and promotes relaxation
Provides stimulation and interest in nature and the outdoors
Improves the sense of wellbeing due to increased social interaction.
There are many different types of dementia gardens, such as healing gardens, sensory gardens and meditation gardens, as well as mobility gardens, rehabilitation gardens and community gardens. Each of these types of gardens can be useful for dementia patients and you should consider the therapy goals and daily therapeutic programs, such as physiotherapy, occupational therapy and horticultural therapy, when you design your garden.
Whichever type of space you are trying to create, the principles and tips below can be a great guide to helping you achieve a wonderful design that meets the needs of the patients.
Design Principles.
The following design principles have been specifically developed with the needs of individuals and groups with dementia in mind. They have been written to help you to consider the variety of decisions that should be made at the planning stage of your garden and will help to maximise the use and benefits of dementia gardens.
Sustainability
For any garden, especially dementia gardens, it is important for the design and upkeep to be sustainable. If the garden falls into disrepair it will become under-utilised and unsafe for both users and staff.
The staff should not be expected to maintain the space, their focus should be on caring for their patients and it is also unlikely that they will have the time to ensure the facility is well kept. Depending on the size and complexity of the space, make sure that you hire a regular maintenance contractor or specialised staff member to care for outdoor spaces.
Gardens will be more sustainable if they are carefully planned from the outset.
Orientation
As mentioned above, dementia patients have a number of symptoms that need to be catered for in a garden. Providing a well-laid-out garden that is properly planned from the beginning can assist users to feel comfortable in using the space and minimise the potential for disorientation and distress in navigating their way in the garden.
Gardens that have areas with clearly defined roles and include indicators for direction and location allow users to behave and use the space more independently. For example, designing your garden to have paths that loop back to the beginning will still allow patients to journey through the landscape without risk of becoming lost.
Accessibility
Gardens need to be accessible for both patients and staff if they are to receive regular use. Dementia patients frequently have health issues associated with ageing, as well as other issues of mobility to consider.
Careful thought, planning, design and implementation will help users to maximise their independence in the landscape, encourage physical activity and allow the users to decide how they would like to interact with the outdoor space.
Considering issues associated with climate and weather can also make a garden more accessible. Create covered outdoor spaces for enjoyment of the garden in inclement weather. Use screens to help reduce the effects of wind and sun. Create transitional spaces between indoors and outdoors to give patient’s eyes time to adjust. Plant carefully placed canopies in parts of the garden to allow for dappled sunshine or times of full shade and cool relaxation.
Socialisation and solitude
One of the main benefits of gardens for dementia patients is the increased socialisation opportunities they create. Users can have greater opportunities for enjoying relaxed, regular, social interaction in an outdoor setting with other patients and staff, as well as with family and friends.
Gardening lends itself easily to interacting with communicatively challenged individuals. It can help to promote teamwork, self-esteem and self-confidence, particularly through regular social interaction. It is also helpful for decision-making skills and providing a feeling of self-determination and control.
Just as dementia patients can have the need for greater social interaction, they can also be living in close quarters with many other people and often feel the need for some private time alone. Achieving an appropriate garden layout that allows for staff supervision for safety, balanced with quieter places for solitude can help to meet this need.
Meaningful activity
There are many, many ways that gardens can help dementia patients to increase the meaningful activity in their lives.
Planning a garden that caters to the therapy needs of patients will help regular care staff and other staff, such as therapists, to make use of the outdoor spaces you design. Providing well maintained, accessible spaces creates ready-made opportunities for staff to tap into when caring for patients. This can be as simple as, ‘Why don’t we take a stroll and look at the changing colours of the leaves in the garden?’, but it can also provide opportunities for more structured activities associated with horticultural therapy, for example.
Planting an array of flowers that can be used for flower arranging or providing pine trees with cones can allow patients to make and decorate bird feeders.
Consulting with the range of staff who use the facility can make sure that outdoor spaces can be designed in a way that will maximise their use. It can help to determine many key aspects from plant selection to ensuring that storage is organised, accessible and adequate for the equipment that will be used. This will also help to ensure the garden is well-maintained and that patients and visitors can access and care for their own equipment. Explaining the garden design layout and features to staff will also help them to access all its spaces and features and allow them to develop or adapt appropriate activities.
Speaking and consulting with the dementia patients is also a critical part of the design process. It helps to better cater to their individual needs and desired usage for garden and it also fosters a sense of ownership and control. In this way, you can provide opportunities for more meaningful activity in the garden. Gardens have usually been a place of meaningful, everyday activity for most dementia patients and offering a range of normal activities can make the garden feel comfortable and home-like. Examples of this are regular gardening activities such as raking leaves, as well as home duties such as hanging out the washing.
This kind of careful planning will also help to make sure that the garden is used frequently and maximum benefit achieved.
Reminiscence
Stimulating reminiscence in dementia patients can be an excellent way to help maintain mental acuity. Choose garden styles and plants that are familiar and recognisable to dementia patients and reminiscent of an appropriate era. Selecting the right plants and styles can also assist with interaction with staff and visitors as they provide an opportunity for suffers to share their life memories and experiences with others.
Sensory stimulation
Sensory stimulation can be a wonderful way for dementia patients to really enjoy nature and the outdoor spaces you create, whilst for other patients sensory stimulation can lead to sensory overload. Providing a number of different spaces within a garden is a good way to balance this dichotomy. Keep some areas of your garden tranquil with subdued colours and very familiar plant choices but also create spaces that are stimulating to each of the five senses: sight, sound, touch, taste and smell. The sense of smell can also be particularly effective in provoking memories for all people, but especially for individuals with dementia. Select plants with a variety of foliage colours and flowers, plants with different textures, scrumptious herbs, vegetables and fruits for smell and taste, as well as grasses and trees that rustle or crunch. Your plant selections could also reflect the change in seasons.
Including plants and other features that attract wildlife can also help to stimulate the senses. You could try bird baths and feeders, as well as certain plants to attract bird life but you can also consider other kinds of wildlife such as butterflies, earthworms, bees or small marsupials.
Safety balanced with independence
Whilst safety must always be of paramount concern, it is important to the quality of life of dementia suffers for this principle to be balanced with opportunities for independence.
Try to make sure that your garden design and inclusions allow people to use the garden as freely as possible whilst still giving staff adequate ability to supervise patients. Try to make the garden as easily accessible to living spaces as possible to encourage regular movement between indoor and outdoor spaces. Provide a range of activities and different kinds of spaces to allow individuals to choose the different ways they would like to use the space and interact with their natural surroundings.
Dementia Garden Layouts.
When designing a dementia garden, the first consideration will be about the size and shape of the space you need to work with. Tara Graham Cochrane of Designwell developed some excellent garden layouts that can be adapted to suit three different types of spaces:
A large garden
A narrow garden, and
A small inner courtyard garden.
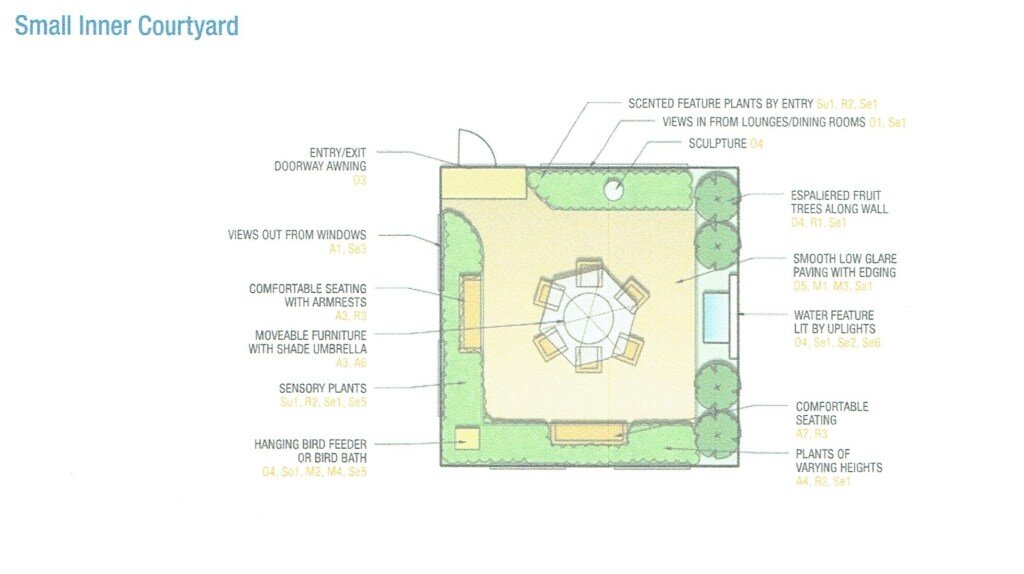
In looking closely at these layouts, you will notice that they are sustainable designs with inclusions for safety, orientation and accessibility, looped paths, features for providing meaningful activity and a variety of different areas for a range of activities and ways of interacting with nature and the outdoor space. Sensory and edible plant features have also been included.
Large Garden Example
Narrow Garden Example
Small Courtyard Example

Get in touch.
Reach out to find out more about designing and building a Dementia Garden, we’d love to chat.